Cataract surgery is a procedure to remove the lens of the eye and, in most cases, replace it with an artificial lens. A cataract causes the lens to become cloudy when it is typically clear. Cataracts can eventually affect vision. Cataract surgery is performed by an eye doctor, also called an ophthalmologist.
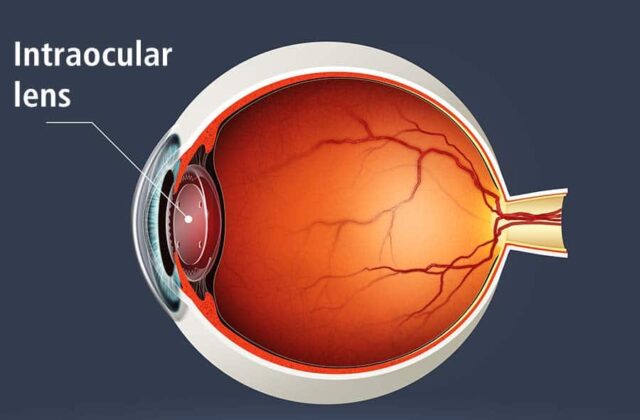
Cataract surgery replaces the cloudy lens inside the eye with an artificial lens. Cataracts are common as you age, and surgery is usually safe and effective. Depending on your replacement lens, you may need glasses after cataract surgery.
It's normal to have:
- grittiness
- watering
- blurred vision
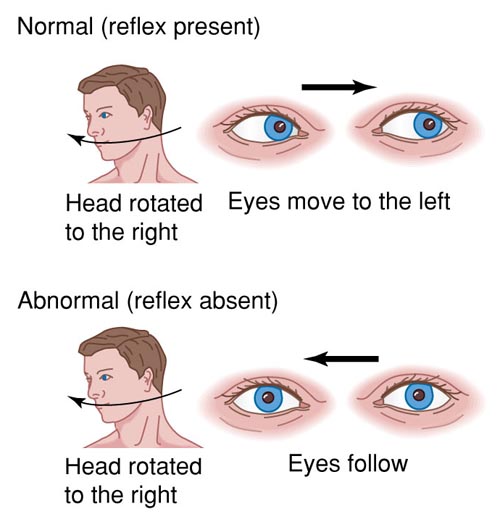
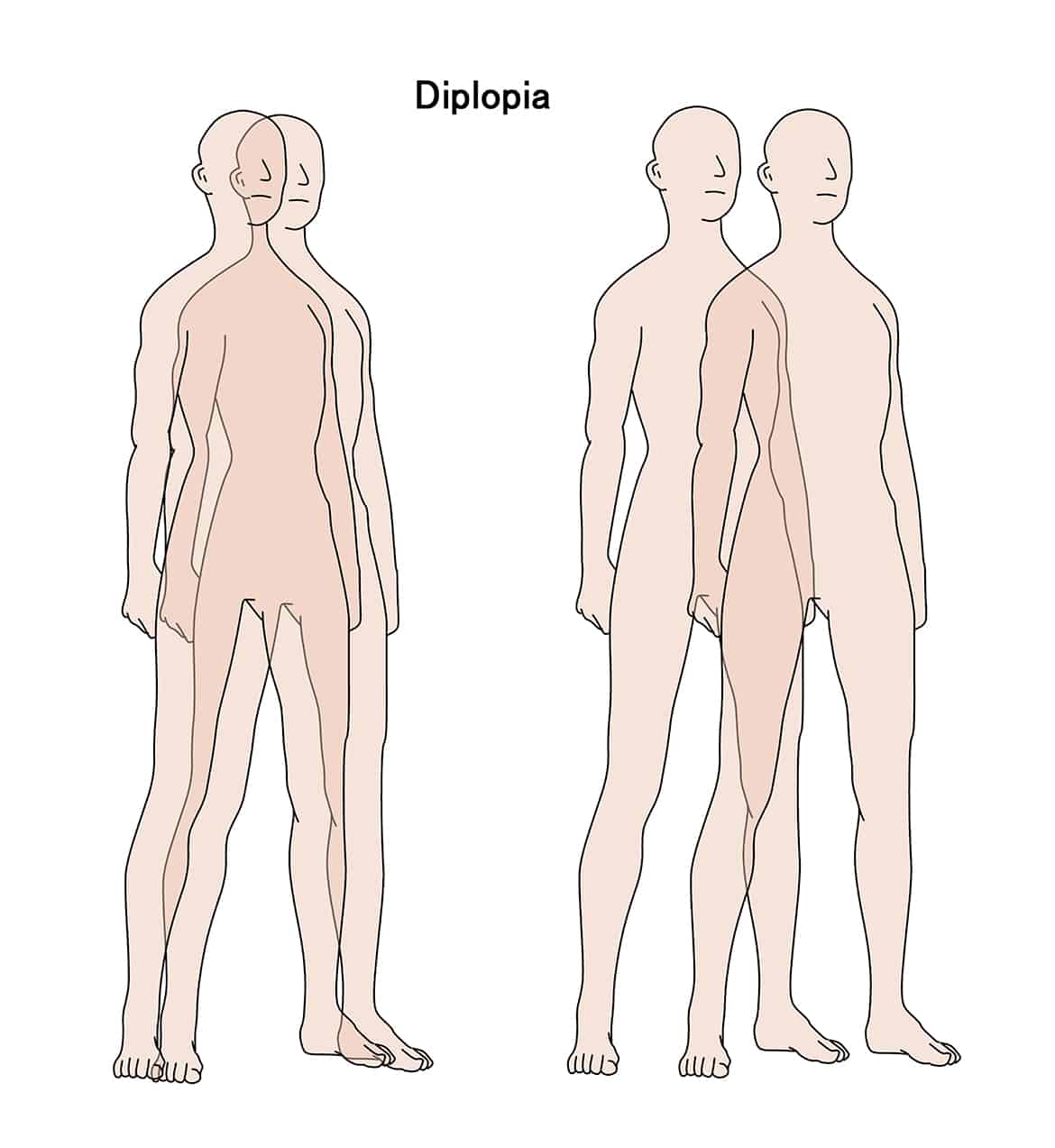
- double vision
- a red or bloodshot eye
These side effects usually improve within a few days, but it can take 4 to 6 weeks to recover fully.
For the first few weeks after surgery:
Do:
- use your eye drops as instructed
- take it easy for the first 2 to 3 days
- use your eye shield at night for at least a week
- take painkillers if you need to
- bathe or shower yourself as usual
- wear your eye shield when washing your hair
- read, watch TV and use a computer
- use your shield, old glasses or sunglasses outdoors
- avoid swimming for 4 to 6 weeks
What should you not do after a cataract operation?
Don't:
- do not rub your eyes.
- do not allow soap or shampoo to get into your eye.
- do not drive until you get the all-clear from your doctor.
- do not do any strenuous exercise or housework.
- do not wear eye make-up for at least 4 weeks.
- do not fly without seeking advice from your doctor.
Which glasses are best after cataract surgery?
Polarized lenses – Shop for cataract surgery sunglasses with polarized lenses, which reduce glare and are especially good for driving, says Dr. Khan. “They're going to give you a crisper image, and that comes in handy any time clarity of vision is important,” she says.

Who needs glasses after cataract surgery?
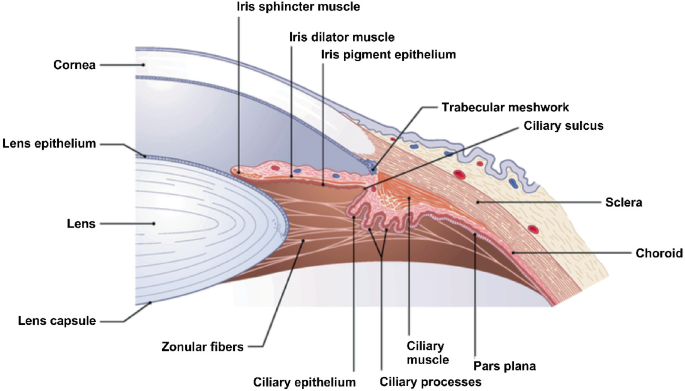
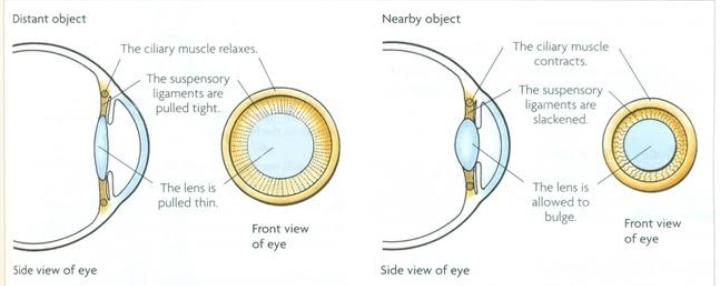
The lens is a curved piece of clear tissue in your eye. Situated behind your pupil, it changes the way light enters your eye and helps you focus your vision at different distances.
Cataract surgery involves replacing the lens in your eye with an artificial replacement called an intraocular lens (IOL). Whether you’ll need glasses after cataract surgery largely depends on what type of IOL you get.
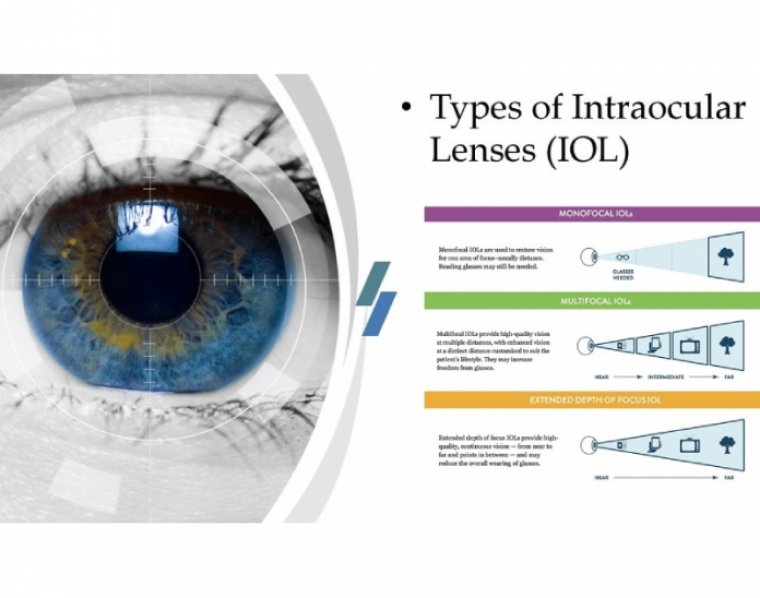
There are many IOL options. Take the time to talk with your eye surgeon beforehand so that you make the choice that’s right for you
The main types of IOLs include:
- Monofocal: Monofocal IOLs are the most common, and also the only IOL that is usually covered by Medicaid and private health insurance. They focus at only one distance, either close, far, or intermediate range. Most people get them for distance vision.
- Multifocal: Multifocal IOLs provide both distant and near focus at the same time. They contain different zones, shaped like concentric rings, that allow you to focus on objects far away as well as objects close up.
- Extended depth of focus: Extended depth of focus IOLs have only one corrective zone. This zone is stretched to allow distance and intermediate vision.
- Accommodative: Accommodative IOLs change shape like your eye’s natural lens to allow you to focus at different distances.
- Toric: Toric IOLs correct astigmatism, a vision issue that’s caused by an irregularly shaped cornea.
- Light-adjustable lens (LAL): This newer type of IOL is the only one that can be customized after surgery. Adjustments are done through a series of office-based light treatment procedures.
How long should you wait before getting new prescription glasses after cataract surgery?
It’s important to wait for your eyes to fully heal and your vision to stabilize before getting a new prescription. Eye doctors often recommend waiting around 6 weeks after your surgery before having your eyes tested and getting new glasses.
Are there any signs that indicate you need new glasses?

It’s typical to have some blurriness and trouble seeing for a few days after cataract surgery. If you notice persistent changes to your vision, you may need to change your prescription.
Some vision changes you might notice include:
- blurry vision
- squinting a lot
- tired eyes
- frequent headaches
- light sensitivity
How do you know which glasses are right for you?
After you’ve healed from your cataract surgery, your eye doctor will perform an updated refraction to determine which eyeglass prescription is best for you. It’s most common that people who undergo cataract surgery will need reading glasses after their vision has stabilized.
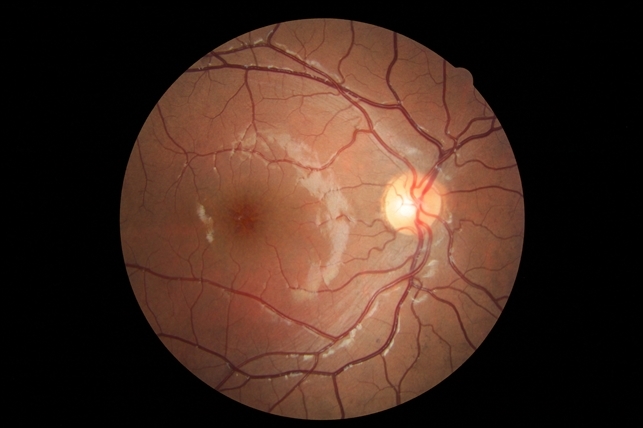
CME (Cystoid macular edema) is the most frequent complication after an uncomplicated cataract surgery.
What are the negatives of cataract surgery?
Is there a downside to having cataract surgery? While generally safe and effective, cataract surgery carries risks like any surgery, including infection, swelling, and vision issues. However, serious complications are rare.
Reference:
- healthline.com/health/eye-health/glasses-after-cataract-surgery#when-glasses-are-needed
- glaucoma.org/articles/premium-intraocular-lenses-iols-for-patients-with-glaucoma
- practiceplusgroup.com/knowledge-hub/risks-benefits-cataract-surgery
- eyewiki.org/Cataract_Surgery_Complications
- nhs.uk/conditions/cataract-surgery/recovery
See also:













:max_bytes(150000):strip_icc()/Parents-Blurry-Vision-Pregnancy-207bb2797209420d915dc2ccc4f57ba8.jpg)








 وبلاگ تخصصی عینک شامل مجموعه مطالب پزشکی است که اطلاعات مفیدی در رابطه با عینک , چشم، لنز، سلامتی چشم و راه های پیشگیری از بیماریهای چشمی، کنترل و درمان آن را در اختیار شما کاربر محترم می گزارد.
وبلاگ تخصصی عینک شامل مجموعه مطالب پزشکی است که اطلاعات مفیدی در رابطه با عینک , چشم، لنز، سلامتی چشم و راه های پیشگیری از بیماریهای چشمی، کنترل و درمان آن را در اختیار شما کاربر محترم می گزارد.